This past weekend I received several messages related to pelvic floor dysfunctions that are not being taken at face value. “Well you’ve had kids”, “it’s all in your head”, “this is a psychosocial problem not a physical problem”. I have said it before and I will say it again, women need to be listened to, trusted, and most importantly, respected when they bring problems to healthcare providers, family, and friends. Although it may seem helpful to say that “this is something that happens when you have had kids”, it can be less than helpful AND is often not the case.
Pelvic Organ Prolapse (POP), is becoming a more well known topic of discussion in various mom groups, and in particular postpartum fitness groups. A large part of the impression I get as I am tagged, mentioned, and participating in these various forums is there seems to be significant panic associated with POP. People become paralyzed, hyper vigilant, and fearful of movement (also known as Kinesiophobia). So let’s break it down to dispel some of the hysteria that seeps into many pelvic health related issues.
Your top three organs that prolapse are (typically) your bladder (cystocele), your rectum (rectocele), and your uterus (uterine prolapse). Although most commonly occurring after child-birth, even those without children can have POP. Let’s focus on pregnancy and post-partum phase.

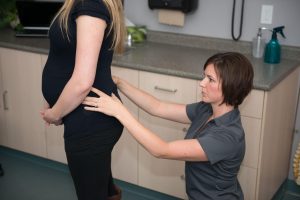
During pregnancy your uterus grows from approximately 5cm in size (which would hang out below your pubic bone), to what seems impossibly large to house the tiny little growing miracle (all the way up to the rib cage). This feat in and of itself does a few things, but thinking of organs specifically – they get moved, pushed and pressed all over the place because there just isn’t room.
How is this possible? Imagine your organs are like little boats at the dock. The boats (organs) wouldn’t do well in inclement weather (movement) if they were tied tightly or cemented to the dock; instead they have ropes (ligaments) to attach and hold them in a relatively stable position relative to the dock (abdominal wall/pelvis/ribs), and the other boats. Your organs aren’t cemented in place either, they essentially float being guided by ligaments, general positioning and support from other organs and the pelvic floor, as well as all the other connective tissue. So, when you are pregnant and the uterus is forging its way through the pelvic and abdominal cavity, everything else is able to move into new positions to compensate.

Once baby is born (vaginal or C-section), the organs suddenly have a lot more space to move around in – their ligaments and fascia have stretched, and there is no longer a tiny human occupying the extra space. As everything settles into a ‘new normal’, if everything is coordinating well, the organs will be situated in a similar position to pre-pregnancy with some slight variance. If the pelvic floor isn’t able to support, or other muscles around the rib cage are having difficulty relaxing, we can get changes in pressure that contribute to pushing these organs down and create POP and various symptoms.
What do we watch for? Feeling of heaviness, falling down or falling out, pressure, discomfort, or bulging, difficulty inserting a tampon, or keeping a tampon in, are all common complaints of POP.
There is much that Pelvic Floor Physio can do to assist with POP, and in many instances resolution of symptoms is possible.

 Haylie has been practicing women’s health and focused in prenatal and post-partum care since graduating from the U of S MPT program in 2011. Advocating for treatment for women, ensuring appropriate and effective care throughout pregnancy and post-partum, and helping all expecting and post-partum moms brought her to open her family-friendly clinic; where clients are encouraged to bring their infants and children to treatment. Warman Physiotherapy & Wellness has been nominated for the 2016 WMBEXA and ABEX Awards, is a WMBEXA award recipient of 2017, and Haylie was recognized as YWCA Women of Distinction for Health & Wellness in 2017.
Haylie has been practicing women’s health and focused in prenatal and post-partum care since graduating from the U of S MPT program in 2011. Advocating for treatment for women, ensuring appropriate and effective care throughout pregnancy and post-partum, and helping all expecting and post-partum moms brought her to open her family-friendly clinic; where clients are encouraged to bring their infants and children to treatment. Warman Physiotherapy & Wellness has been nominated for the 2016 WMBEXA and ABEX Awards, is a WMBEXA award recipient of 2017, and Haylie was recognized as YWCA Women of Distinction for Health & Wellness in 2017.